
Chronic inflammatory demyelinating polyradiculoneuropathy; Polyneuropathy - chronic inflammatory; CIDP; Chronic inflammatory polyneuropathy; Guillain-Barré - CIDP
Chronic inflammatory demyelinating polyneuropathy (CIDP) is a disorder that involves nerve swelling and irritation (inflammation) that leads to a loss of strength or sensation.
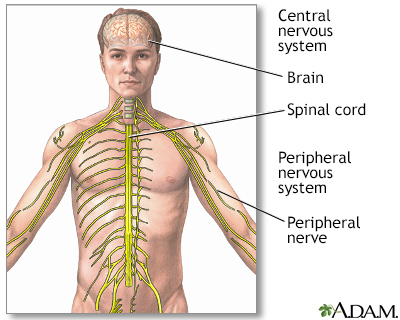
CIDP is one cause of damage to nerves outside the brain or spinal cord (peripheral neuropathy). Polyneuropathy means several nerves are involved. CIDP often affects both sides of the body.
CIDP is caused by an abnormal immune response. CIDP occurs when the immune system attacks the myelin cover of the nerves. For this reason, CIDP is thought to be an autoimmune disease.
Health care providers also consider CIDP as the chronic form of Guillain-Barré syndrome.
The specific triggers of CIDP vary. In many cases, the cause cannot be identified.
CIDP may occur with other conditions, such as:
Symptoms include any of the following:
Other symptoms that can occur with CIDP include:
The provider will perform a physical exam and ask about the symptoms, focusing on the nervous system and muscles.
Tests that may be ordered include:
Depending on the suspected cause of CIDP, other tests, such as x-rays, imaging scans, and blood tests, may be done.
The goal of treatment is to reverse the attack on the nerves. In some cases, nerves can heal and their function can be restored. In other cases, nerves are badly damaged and cannot heal, so treatment is aimed at preventing the disease from getting worse.
Which treatment is given depends on how severe the symptoms are, among other things. The most aggressive treatment is only given if you have difficulty walking, breathing, or if symptoms don't allow you to care for yourself or work.
Treatments may include:
The outcome varies. The disorder may continue long term, or you may have repeated episodes of symptoms. Complete recovery is possible, but permanent loss of nerve function is not uncommon.
Complications of CIDP include:
Contact your provider if you have a loss of movement or sensation in any area of the body, especially if your symptoms get worse.
Katirji B. Disorders of peripheral nerves. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 106.
Smith AG, Shy ME. Peripheral neuropathies. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 388.
BACK TO TOPReview Date: 6/13/2024
Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

|
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.