
Skeletal survey
A skeletal x-ray is an imaging test used to look at your bones. It is used to detect fractures, tumors, or conditions that cause wearing away (degeneration) of the bone.

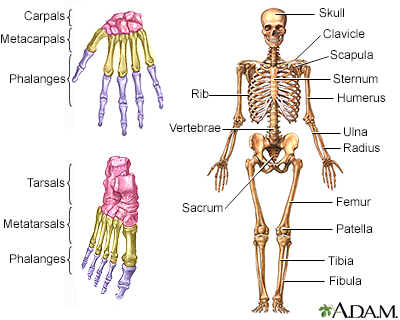
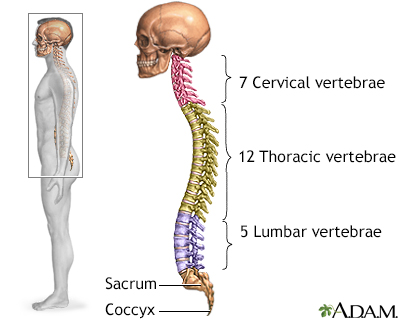

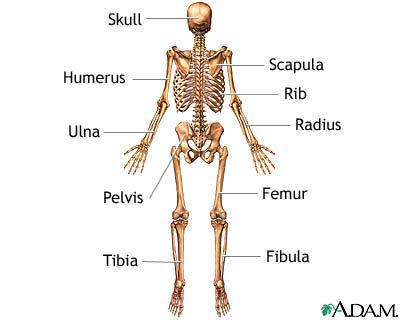
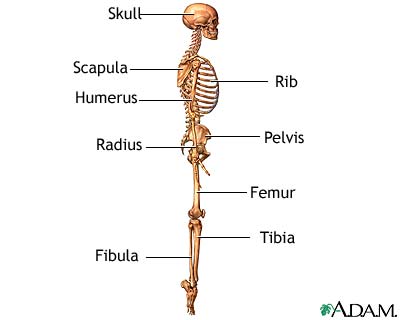

The test is done in a hospital radiology department or in your health care provider's office by an x-ray technologist.
You will lie on a table or stand in front of the x-ray machine, depending on the bone that is injured. You may be asked to change position so that different x-ray views can be taken.
The x-rays pass through your body. A computer or special film records the images.
Structures that are dense (such as bone) will block most of the x-ray particles. These areas will appear white. Metal and contrast media (special dye used to highlight areas of the body) will also appear white. Structures containing air will be black. Muscle, fat, and fluid will appear as shades of gray.
Tell your provider if you are pregnant. You must remove all jewelry before the x-ray.
The x-rays are painless. Changing positions and moving the injured area for different x-ray views may be uncomfortable. If the whole skeleton is being imaged, the test most often takes 1 hour or more.
This test is used to look for:
Abnormal findings include:
There is low radiation exposure. X-rays machines are set to provide the smallest amount of radiation exposure needed to produce the image. Most experts feel that the risk is low compared with the benefits.
Children and the fetuses of pregnant women are more sensitive to the risks of the x-ray. A protective shield may be worn over areas not being scanned.
Contreras F, Perez J, Jose J. Imaging overview. In: Miller MD, Thompson SR, eds. DeLee, Drez, & Miller's Orthopaedic Sports Medicine. 5th ed. Philadelphia, PA: Elsevier; 2020:chap 7.
Kapoor G, Toms AP. Current status of imaging of the musculoskeletal system. In: Adam A, Dixon AK, Gillard JH, Schaefer-Prokop CM, eds. Grainger & Allison's Diagnostic Radiology. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 38.
BACK TO TOPReview Date: 4/1/2025
Reviewed By: Linda J. Vorvick, MD, Clinical Professor Emeritus, Department of Family Medicine, UW Medicine, School of Medicine, University of Washington, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

|
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.